Understanding the source of your foot pain is the key to finding lasting relief. For many, that source is Plantar Fasciitis, an inflammation of the ligament connecting your heel to your toes. This vital tissue acts as a shock absorber, but repetitive stress from standing on hard surfaces, wearing unsupportive shoes, or even a sudden increase in activity can cause painful micro-tears. This guide breaks down the mechanics behind Plantar Fasciitis, helping you understand why it happens. We will also provide actionable tips, from at-home exercises to the critical role that supportive orthotics and footwear play in your recovery and prevention of future flare-ups.
Plantar fasciitis is a common type of inflammation that occurs when the plantar fascia is excessively stretched. The plantar fascia is a band of fibrous tissue that runs along the bottom surface of the foot that connects each of the toes with part of the heel bone. Every time your foot strikes the ground, the plantar fascia is stretched. The pain is commonly felt in the arch and heel in one or both feet, usually worst in the morning during the first few steps or after sitting for a long period of time time.
CAUSES OF PLANTAR FASCIITIS
Plantar fasciitis results from long-term pressure and excessive strain on the foot. The lead cause of plantar fasciitis is overpronation, or flat feet, which results when the ankle rolls inward and the arch collapses upon weight bearing, causing the plantar fascia to stretch away from the heel.
Other Common Causes:
- Structural foot setbacks like high arches
- High impact activities like running, dancing, or jumping
- Sudden increase in exercise or physical activity
- Sudden weight gain such as obesity or pregnancy
- Standing or walking on hard floors for long periods of time
- Ill-fitting shoes
SYMPTOMS OF PLANTAR FASCIITIS
Plantar fasciitis feels like a stabbing or aching heel pain when you take your first steps in the morning. It can often lead to arch pain; if left untreated and the strain on feet continues, a heel spur may develop. Do you have foot pain? Take the Aetrex Orthotic Quiz to find out what kind of insoles work best for you.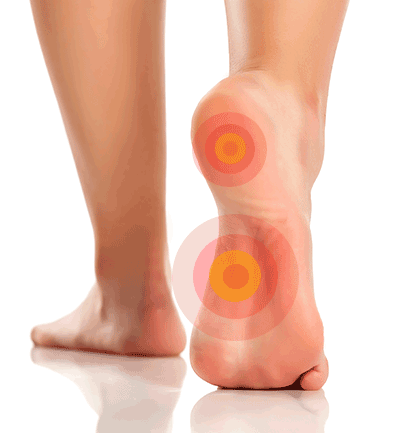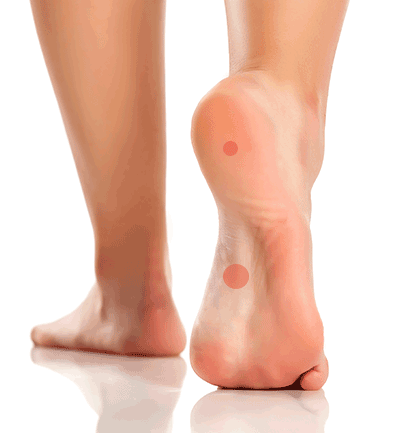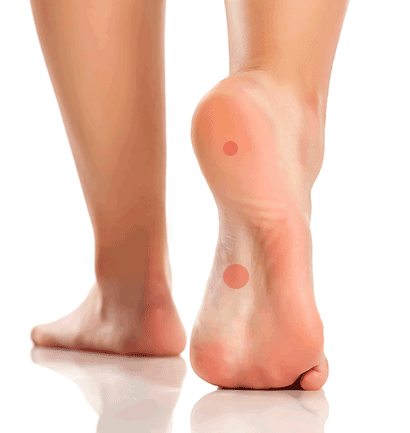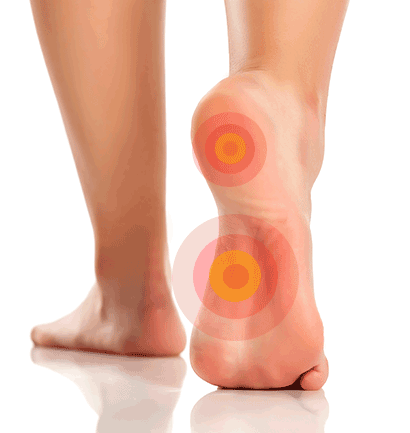
PEDIATRIC PLANTAR FASCIITIS
Just like adults, children can also develop plantar fasciitis from the excessive stretching of the plantar fascia. Children who participate in sports and high-impact activities are more likely to develop plantar fasciitis.
Additional Causes:
- Improper stretching
- Tight calf muscles
- Sudden weight gain
- Ill-fitting shoes
PREVENTION OF PLANTAR FASCIITIS
There are many ways to support your feet to avoid developing plantar fasciitis. If you stand all day at work or walk on hard services, it's imperative to have proper arch and heel support in your shoes/orthotics.
- Avoid running on hard or uneven ground
- Wear orthotics that support your arches and heel
- Wear shoes with proper arch support
- Avoiding wearing high-heeled shoes
- Maintain a healthy weight
TIPS FOR TREATING PLANTAR FASCIITIS
If you are feeling pain from plantar fasciitis, try these tips for relief.
- Choose footwear and orthotics that support your feet
- Avoid walking on hard surfaces
- Stretch the feet and calves
- Massage the feet
- Ice the area 10-20 minutes at a time, up to 3 times per day
- Rest
10 SIMPLE PLANTAR FASCIITIS EXERCISES TO RELIEVE PAIN
Here are a few exercises that will keep your feet strong and help reduce foot & ankle pain. These exercises only take a few minutes and can simply be done at home. Make sure you maintain proper posture by sitting up straight for the exercises that require sitting in a chair.
1. Towel Curls
Sit down in a chair with your heels under your knees. Place your feet flat at the end of the towel and use your toes to pull the other end of the towel towards you. Make sure your heel stays where it is while you move a little bit of towel each time you extend and pull back. Repeat 4-5 times and move in the opposite direction.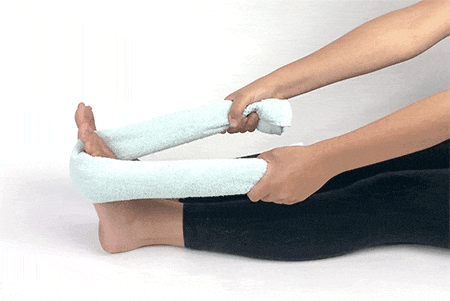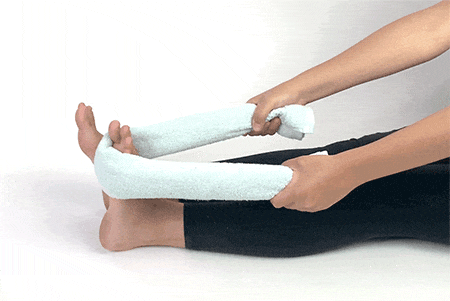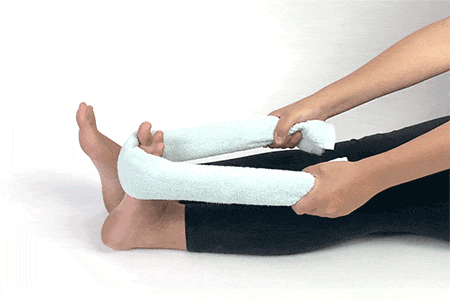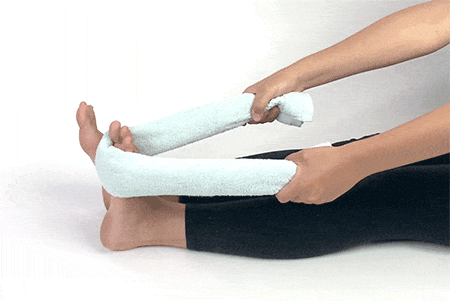
2. Ball Roll
Sit on a chair and place a tennis ball on the floor near your feet. Move your foot on top of the tennis ball and roll it around the ball. Use the ball to massage the bottom of your foot for 3-5 minutes. You can increase or decrease the pressure on the tennis ball as needed.
3. Frozen Bottle Roll
Place a bottle of water in the freezer until it turns into ice. Roll the frozen bottle under your foot similar to a ball roll. This helps reduce inflammation.
4. Marble Pick Ups
Place marbles and a cup on the floor. Use your toes to pick up one marble and slowly place it in the cup. Repeat it 7-8 times on each foot.
5. Ankle Circles
Sit up straight on a chair and lift your foot to draw circles using the big toe. Draw circles using your big toe clockwise and anticlockwise.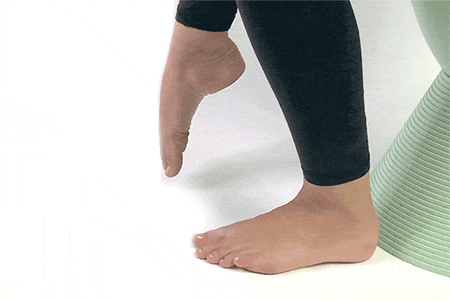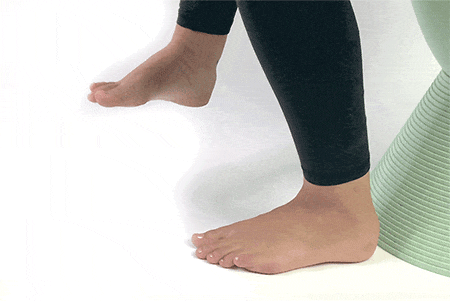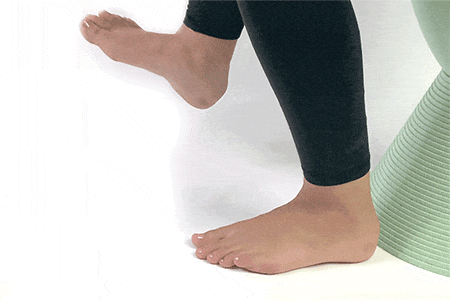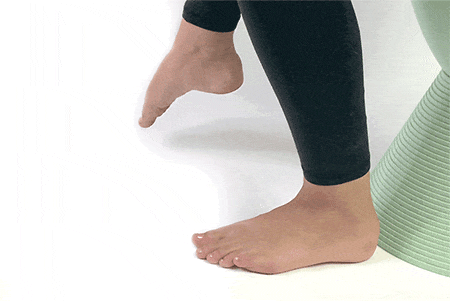
6. Heel Raises
Stand up straight and place your hands on the back of a chair for support. Raise your heels and try to stand on your toes to stretch your arch. Hold this position for 10-20 seconds and lower your heels back down slowly. If you can hold your balance, try the same exercise on a step.
7. Towel Stretch
Sit up straight on the ground with your legs extended and knees straight. Place a folded towel around your foot and gently pull it towards you. Hold it for 15-20 seconds and repeat 3-4 times on each foot.

8. Big Toe Stretch
Sit up straight on a chair and cross one leg over the other. Make sure your other foot is flat on the ground. Hold your big toe with your fingers and gently move it toward you and away from the other toes. Hold this stretch for 15 seconds and move it in the opposite direction for 15 seconds. You can repeat this 3-4 times on each foot.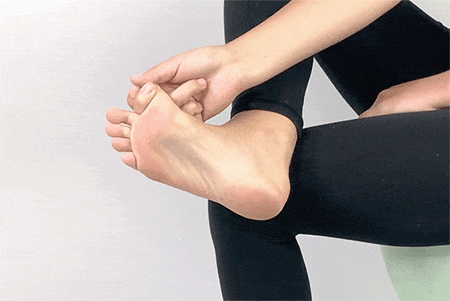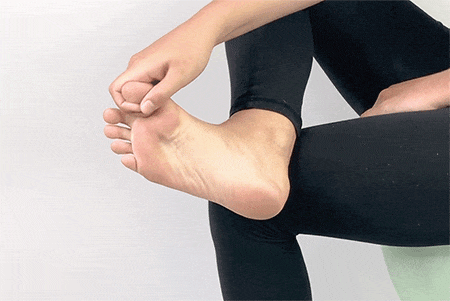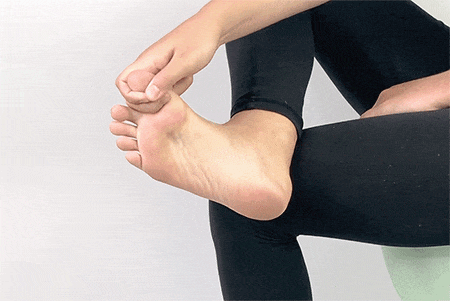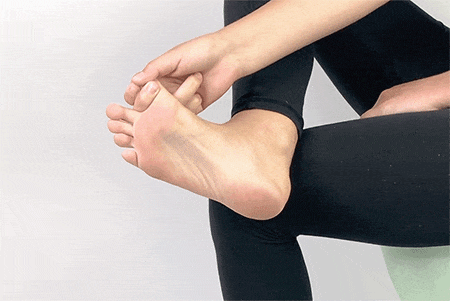
9. Toe Splay
Sit up straight on a chair and place your feet flat on the ground. Spread your toes away from each other and hold the stretch for 5-7 seconds and release. Repeat 5-6 times.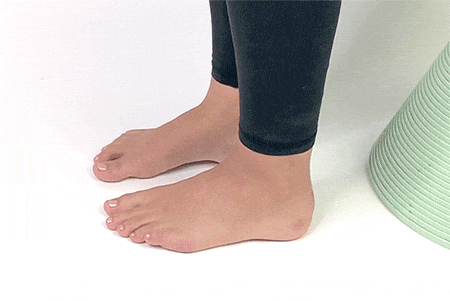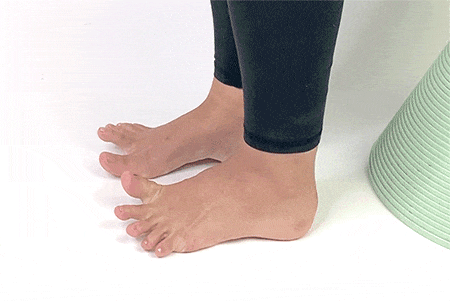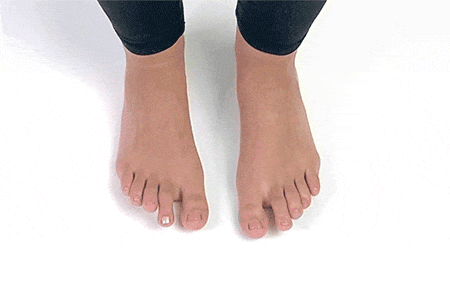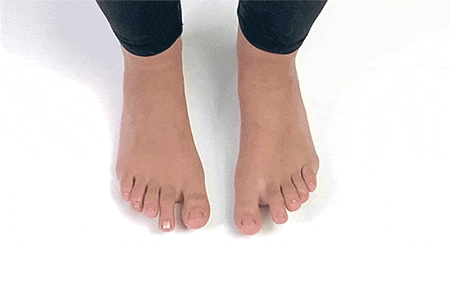
10. Calf Stretch
Stand facing a wall, about one and a half foot lengths away. Place both hands on the wall at shoulder height. Your arms should be outstretched; adjust your feet as necessary. With your feet pointing straight ahead, place one foot in the back of the other. The front leg should have a bent knee and the leg behind it should have a straight knee. Gently bend forward with your right heel on the ground. Hold for the stretch for 15-30 seconds and reverse the position of your legs to repeat the stretch.
HOW TO CHOOSE THE BEST ORTHOTICS FOR PLANTAR FASCIITIS
Orthotics can help relieve plantar fasciitis by cradling the foot and minimizing the repeated stress on the plantar fascia; helping decrease inflammation and pain. There are two important features an orthotic needs to include to help alleviate plantar fasciitis: arch support and heel support. A combination of these features will help prevent the stretching of the plantar fascia. The correct orthotics will help provide extra comfort and reduce the amount of shock and force placed on feet during everyday activities.
Aetrex Orthotics Features:
- Signature Aetrex arch support helps align your body correctly
- Posted heel helps control balance and prevent injuries
- Memory foam for extra cushioning
- Helps provide equal distribution of pressure

The Signature Aetrex arch support is strategically placed further back to provide the right balance and support to the most weight-bearing part of the body and it provides a strong foundation for the plantar fascia to help keep it from stretching which usually occurs when you stand or walk.
What is Plantar Fasciitis?
If you've ever woken up and felt a sharp, stabbing pain in your heel with your first few steps, you might be familiar with plantar fasciitis. It’s one of the most common causes of heel pain, and it happens when the plantar fascia gets inflamed. The plantar fascia is the thick, web-like band of tissue that runs across the bottom of your foot, connecting your heel bone to your toes. Think of it as your foot's natural shock absorber. It supports the arch of your foot and absorbs stress when you walk. When too much pressure or strain is put on this ligament, small tears can occur, leading to inflammation and that all-too-familiar pain.
The pain is typically at its worst in the morning because the fascia tightens up overnight while you sleep. As you start to move around and stretch it out, the pain might decrease, but it can often return after long periods of standing or after getting up from sitting. While it can be incredibly frustrating to deal with, understanding what’s causing the pain is the first step toward finding relief. The key is to support that inflamed tissue and reduce the strain that’s causing the problem in the first place, allowing it to heal properly and get you back on your feet comfortably.
How Plantar Fasciitis Develops
Plantar fasciitis doesn't just appear overnight; it usually results from long-term pressure and excessive strain on the foot. One of the leading causes is overpronation, which is common in people with flat feet. When your foot overpronates, your ankle rolls inward and your arch collapses as you walk, causing the plantar fascia to stretch away from the heel bone. This repetitive stretching can lead to inflammation and significant pain over time. That’s why finding footwear with the right support is so crucial. Aetrex helps to provide relief for plantar fasciitis by designing shoes and orthotics with signature arch support that helps stabilize the foot and prevent the excessive stretching that leads to discomfort.
How Common is Plantar Fasciitis?
If you're struggling with this type of heel pain, know that you are far from alone. Plantar fasciitis is incredibly common, with about two million people receiving treatment for it every year. It affects people from all walks of life, from athletes who put a lot of stress on their feet to individuals who spend long hours standing on hard surfaces for work. Because it's such a widespread issue, there are many well-established strategies for managing the pain and helping your feet heal. Making simple changes, like choosing supportive footwear and incorporating daily stretches, can make a huge difference in your comfort and mobility.
Plantar Fasciitis vs. Heel Spurs
It's common to hear plantar fasciitis and heel spurs mentioned together, and it’s easy to confuse the two. While they are related, they are not the same condition. A heel spur is a calcium deposit that causes a bony protrusion on the underside of the heel bone. While many people with plantar fasciitis also have heel spurs, the spur itself is not usually the cause of the pain. The discomfort you feel is from the inflammation of the plantar fascia ligament. The focus for relief should be on supporting the inflamed tissue, not the bone spur. Wearing orthotics with deep heel cups and proper arch support helps to cushion the area and reduce stress on the fascia.
Potential Complications of Ignoring Pain
It’s tempting to think that sharp morning heel pain will just go away on its own, but ignoring plantar fasciitis can lead to more significant issues down the road. When you try to avoid the pain in your heel, you naturally change the way you walk. This shift in your gait might offer temporary relief, but it places new stress on other parts of your body, potentially causing secondary pain in your feet, knees, hips, or even your back. Over time, untreated inflammation can also lead to the development of heel spurs, which are bony growths that can cause more discomfort. This creates a difficult cycle where pain reduces your activity levels, affecting your overall health. Addressing the pain early with supportive footwear is a crucial step to prevent these long-term complications and stay active.
Diagnosing Plantar Fasciitis
When to See a Doctor
Trying at-home treatments like stretching, icing, and wearing supportive footwear is a fantastic first step in addressing heel pain. However, if your pain doesn't start to improve on its own after about a week, or if your symptoms are still bothering you after two weeks of consistent self-care, it's a good idea to check in with your doctor. It can be tempting to just push through the discomfort, but ignoring plantar fasciitis can allow it to become a long-term problem that stops you from enjoying your normal activities. Getting a professional diagnosis is key to creating an effective plan to help you find relief and get back to your routine, pain-free.
What to Expect During an Exam
The good news is that diagnosing plantar fasciitis is usually a straightforward process. During your appointment, your doctor will likely start by asking about your medical history and your symptoms—for example, when the pain is most noticeable and what activities seem to trigger it. They will then conduct a physical exam of your foot to check for tenderness, especially along the bottom of your foot and heel, and look for any swelling. Most of the time, this is enough to confirm a diagnosis. Imaging tests like X-rays are rarely needed unless your doctor wants to rule out other potential causes for your pain, such as a bone spur, fracture, or arthritis.
Replace Your Athletic Shoes Regularly
Wearing the right shoes is one of the most important steps you can take for both treating and preventing plantar fasciitis. If you're active, it's a good idea to replace your athletic shoes every six to nine months, or after about 250 to 500 miles of use. Over time, the cushioning and support structures inside your shoes break down, even if they still look fine on the outside. This loss of support means your feet absorb more impact with every step, which can put extra strain on your plantar fascia and lead to that familiar stabbing pain in your heel.
When shopping for new footwear, look for shoes with thick, cushioned soles and prominent arch support. These features help to absorb shock and reduce pressure on your heel. Aetrex Helps to alleviate this pressure by designing every pair of our shoes for plantar fasciitis with our signature arch support built right in. This system is strategically placed to help stabilize your foot, properly align your body, and relieve strain on the plantar fascia, giving you a strong foundation for pain-free movement.
For an extra layer of comfort, you can also add orthotic inserts to your shoes. A high-quality orthotic can provide targeted cushioning and support exactly where you need it most. All Aetrex Orthotics feature our signature arch support combined with premium memory foam to cradle your foot and absorb shock. Using an orthotic helps to distribute pressure evenly across your foot, which can make a significant difference in managing plantar fasciitis symptoms and keeping your feet comfortable all day long.
At-Home Care and Lifestyle Changes
When you're dealing with the persistent pain of plantar fasciitis, finding relief is a top priority. The good news is that many effective strategies can be done right at home. Making a few simple adjustments to your daily routine can significantly reduce strain on your plantar fascia, giving it the chance to heal. These at-home care methods focus on reducing inflammation, alleviating pressure on your feet, and preventing the pain from getting worse. By being proactive and consistent with these changes, you can take control of your recovery and get back on your feet comfortably.
Activity Modification
One of the most important first steps is to rest your feet. This means reducing or even stopping the activities that you know make the pain worse, especially high-impact exercises like running or jumping. This doesn't mean you have to stop being active altogether. Instead, you can swap your usual workout for low-impact exercises like swimming or cycling, which don't put as much stress on your feet. Giving your plantar fascia a break from constant strain is crucial for allowing the inflammation to go down and the healing process to begin.
Over-the-Counter Medication
To manage the immediate pain and swelling, over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can be helpful. These medications can provide temporary relief, making it easier to get through your day. However, it's important to remember that while they address the symptoms, they don't address the underlying cause of the strain on your feet. Think of them as a helpful tool in your recovery toolkit, but not the entire solution. Lasting relief comes from addressing the root issues, like improper foot support.
Advanced Medical Treatments
If you've been diligent with at-home care but the pain just isn't going away, it might be time to talk to your doctor about more advanced medical treatments. These options are typically considered when conservative methods haven't provided enough relief after several months. A healthcare professional can properly diagnose your condition and recommend a more intensive treatment plan tailored to your specific needs. From physical therapy to other medical procedures, these next steps are designed to promote healing and provide more significant pain relief when you need it most.
Physical Therapy
A physical therapist can be an incredible ally in your fight against plantar fasciitis. They can create a personalized program of exercises designed to stretch your plantar fascia and Achilles tendon, as well as strengthen your lower leg muscles. Stronger muscles can better support your arch, which reduces stress on the plantar fascia. In addition to exercises, a physical therapist may use other techniques like massage or ice treatments to help reduce pain and inflammation, guiding you through a structured recovery process.
Night Splints
If you experience intense stabbing pain with your first steps in the morning, a night splint might be a game-changer for you. These devices hold your foot in a flexed position while you sleep, which keeps the plantar fascia and Achilles tendon gently stretched overnight. This prevents the tissue from tightening up while you're resting, which is what causes that sharp morning pain. While it might take a little getting used to, wearing a night splint can be a very effective way to find relief.
Injections and Other Therapies
For persistent pain, your doctor might suggest injections. Cortisone shots are a common option; they are powerful anti-inflammatories that can reduce pain effectively. However, it's important to know that repeated injections can potentially weaken the plantar fascia. Another option is platelet-rich plasma (PRP) injections, which use your own blood to encourage healing without the same risks as cortisone, though this treatment can be more expensive. These are options to discuss thoroughly with your doctor to weigh the pros and cons for your situation.
Surgery: A Last Resort
It's important to know that surgery for plantar fasciitis is very rare. It's typically only considered as a last resort if you've tried multiple nonsurgical treatments for at least 12 months without any significant improvement. Because most people find relief through less invasive methods, the vast majority of individuals with plantar fasciitis will never need to consider surgery. The focus is almost always on conservative treatments that support the foot and allow it to heal naturally.
Recovery Time
Patience is key when it comes to recovering from plantar fasciitis. The healing process is different for everyone and can take anywhere from a few weeks to several months. Consistency with your chosen treatments is what will make the biggest difference. Throughout your recovery, it's essential to wear supportive footwear. Aetrex helps to provide the necessary support with shoes and orthotics that feature our signature arch support, which is designed to align your body and reduce pressure on the plantar fascia. Finding the right support with our Orthotic Finder can be a crucial step in your healing journey and in preventing the pain from returning.
HOW TO CHOOSE THE BEST SHOES FOR PLANTAR FASCIITIS
Unsupportive shoes can worsen the pain of plantar fasciitis. Choosing footwear that support your feet is critical to help alleviate discomfort. The most important feature to keep on the top of the list is proper arch support. Aetrex Shoes have supportive features built-in.
Aetrex Shoe Features:
- Supportive arch
- Superior cushioning helps avoid pain in high-pressure areas
- Adjustable straps
- A firm, but flexible midsole
- Cushioning in the arch and forefoot
- Met bar pod
- Bunion pockets
- Padded heel
Check out our list of the 6 Best Flip Flops for Plantar Fasciitis and our Best-Selling Summer Shoes for Plantar Fasciitis!
Reference: Dr. George Ampat FRCS (Tr & Orth), Consultant Orthopaedic Spinal Surgeon
DISCLAIMER: The information contained on this guide is not provided by medical professionals and is provided for informational purposes only. The information on this guide is not meant to substitute consulting with your podiatrist, doctor or other health care professional. The information available on or through this guide is in no way intended to diagnose, influence treatment or cure any foot or other health problems nor is it a substitute for the services or advice of a podiatrist, physician, or health professional. You should always consult a physician licensed in your state in all matters relating to your health.
Frequently Asked Questions
Why does my heel hurt so much when I first wake up? That sharp morning pain is a classic sign of plantar fasciitis. While you sleep, the plantar fascia ligament on the bottom of your foot tightens up. When you take your first steps, you're suddenly stretching that tight tissue, which causes that familiar stabbing sensation. As you walk around and warm up the ligament, the pain usually lessens, but it can return after you've been sitting for a while.
Can I continue my workout routine with plantar fasciitis? It's best to give high-impact activities like running or jumping a rest while your foot is healing. Continuing these activities can put more strain on the plantar fascia and delay your recovery. You don't have to stop moving completely, though. Consider switching to low-impact exercises like swimming, cycling, or using an elliptical machine. These activities keep you active without putting repetitive stress on your feet.
How long will it take for my foot to feel better? Recovery time really varies from person to person and depends on how consistent you are with your treatment. For some, the pain might improve in a few weeks, while for others, it could take several months. The key is patience and consistency. Sticking with your stretches, wearing supportive footwear, and giving your feet proper rest are the most important steps you can take to help the healing process along.
Do I need special shoes, or will orthotics be enough? Both can be incredibly helpful, and they often work best together. A good orthotic provides targeted arch support and cushioning, which you can place in your existing shoes to reduce strain on the plantar fascia. However, if the shoes themselves are worn out or unsupportive, an orthotic can only do so much. Choosing shoes designed with built-in arch support and a cushioned sole gives your foot a stable and comfortable foundation from the start.
Are heel spurs and plantar fasciitis the same thing? That's a common point of confusion, but they are two different conditions. Plantar fasciitis is the inflammation of the ligament itself. A heel spur is a small, bony growth on the heel bone that can develop over time due to the strain from plantar fasciitis. While many people have both, the pain you feel is almost always caused by the inflamed ligament, not the bone spur. Focusing on supporting the arch and cushioning the heel will help relieve the pressure that causes the pain.
Key Takeaways
- Prioritize Proper Foot Support: Reducing strain on your plantar fascia starts with the right foundation; consistently wear shoes and orthotics that feature significant arch support and a cradling heel cup to help stabilize your foot.
- Combine Stretching with Smart Rest: Simple at-home routines are essential for recovery, so gently stretch your calves and feet daily to maintain flexibility and modify high-impact activities to give the inflamed tissue a chance to heal.
- Adopt Proactive Habits for Lasting Relief: Preventing future flare-ups requires consistency, so make a habit of choosing supportive footwear for all activities and regularly replace athletic shoes once their internal support wears down.


Share:
Do Your Feet Hurt During Your First Steps in the Morning?
10 Tips for Music Festivals Without Killing Your Feet